Preventable Harms
Injection Drug Use-Related Infections in New Jersey
Table of Contents
Dedication
Acknowledgments
Acronyms Used
- ED: Emergency Department
- HCUP: Healthcare Cost and Utilization Project
- HIV: Human Immunodeficiency Virus
- ICD: International Classification of Diseases
- IDU: Injection drug use
- IQR: Interquartile range
- NJHRC: New Jersey Harm Reduction Coalition
- PWID: People who inject drugs
- SBI: Severe bacterial infection
- SEDD: State Emergency Department Databases
- SID: State Inpatient Databases
- SSTI: Skin and soft tissue infection
- SUD: Substance Use Disorder
Executive Summary
- 1,967 emergency room visits for IDU-SBIs
- 7,310 hospitalizations for IDU-SBIs, accounting for 0.8% of all hospitalizations and 15.2% of hospitalizations for patients with an injection-related substance use disorder (SUD) diagnosis (SUD) diagnosis
- 283 deaths from IDU-SBIs
- More than $1 billion in hospital charges due to IDU-SBIs, with a median charge of $74,406 per hospitalization
Introduction
Methods
Results
Overall Findings
283 people died from injection drug use-related infections while hospitalized in New Jersey in 2019.
FIGURE 1
Frequency of IDU-SBIs across hospital visits*
*Sum of individual SBIs greater than total number of identified SBI hospitalizations because visits could contain more than one SBI
Prevalence of Severe Bacterial Infections
Demographic Trends
Black/non-Hispanic residents were 1.5 times more likely to be hospitalized than their white counterparts.
People with Medicare or Medicaid were 5.6 times more likely to be hospitalized than those with private insurance.
TABLE 1
Frequencies of IDU-SBI hospitalizations across demographic characteristics†
| Characteristic | Frequency | Percent | N* |
|---|---|---|---|
| SEX | 7,310 | ||
| Male | 4,296 | 58.8 | |
| Female | 3,014 | 41.2 | |
| AGE | 7,310 | ||
| <21 years old | 50 | 0.7 | |
| 21-29 years old | 874 | 12.0 | |
| 30-49 years old | 3,143 | 43.0 | |
| 50-64 years old | 2,301 | 31.5 | |
| 65 years and older | 942 | 12.9 | |
| RACE/ETHNICITY | 7,233 | ||
| White/Non-Hispanic | 4,492 | 62.1 | |
| Black/Non-Hispanic | 1,560 | 21.6 | |
| Hispanic | 861 | 11.9 | |
| Asian/Pacific Islander & Native American | 48 | 0.7 | |
| Other | 272 | 3.8 | |
| PATIENT LOCAL INCOME QUARTILE** | 7,240 | ||
| First Quartile | 3,266 | 45.1 | |
| Second Quartile | 1,981 | 27.4 | |
| Third Quartile | 1,309 | 18.1 | |
| Fourth Quartile | 684 | 9.5 | |
| EXPECTED PAYER‡ | 7,310 | ||
| Medicare | 1,687 | 23.1 | |
| Medicaid | 3,036 | 41.5 | |
| Private Insurance | 1,891 | 25.9 | |
| Self-Pay | 336 | 4.6 | |
| Other | 360 | 4.9 |
†Characteristics are across visits, not individuals.
*Total N varies based on available data from HCUP (Max N =7,310).
**Patient local income quartile calculated based on identified patient’s home zip code.
‡Self-pay includes self-pay, no charge, and no expected payment. Other includes Worker’s Compensation, & other government programs.
IDU: Injection drug use
TABLE 2
Frequency of SBI hospitalizations in 2019 by NJ County*
| County | SBI Encounters | Total Encounters | Total Population | Morbidity per 1,000 Encounters | Morbidity per 1,000 Individuals |
|---|---|---|---|---|---|
| Atlantic | 497 | 34,239 | 263,670 | 14.52 | 1.88 |
| Bergen | 347 | 76,983 | 932,202 | 4.51 | 0.37 |
| Burlington | 375 | 45,475 | 445,349 | 8.25 | 0.84 |
| Camden | 971 | 59,772 | 506,471 | 16.25 | 1.92 |
| Cape May | 88 | 11,490 | 92,039 | 7.66 | 0.96 |
| Cumberland | 201 | 19,791 | 149,527 | 10.16 | 1.34 |
| Essex | 875 | 86,861 | 798,975 | 10.07 | 1.1 |
| Gloucester | 319 | 26,160 | 291,636 | 12.19 | 1.09 |
| Hudson | 471 | 62,043 | 672,391 | 7.59 | 0.7 |
| Hunterdon | 48 | 11,248 | 124,371 | 4.27 | 0.39 |
| Mercer | 405 | 37,657 | 367,430 | 10.75 | 1.1 |
| Middlesex | 335 | 75,865 | 825,062 | 4.42 | 0.41 |
| Monmouth | 374 | 66,116 | 618,795 | 5.66 | 0.6 |
| Morris | 189 | 42,631 | 491,845 | 4.43 | 0.38 |
| Ocean | 469 | 79,235 | 607,186 | 5.92 | 0.77 |
| Passaic | 498 | 53,736 | 501,826 | 9.27 | 0.99 |
| Salem | 79 | 7,037 | 62,385 | 11.23 | 1.27 |
| Somerset | 137 | 25,718 | 328,934 | 5.33 | 0.42 |
| Sussex | 93 | 14,804 | 140,488 | 6.28 | 0.66 |
| Union | 253 | 53,875 | 556,341 | 4.7 | 0.45 |
| Warren | 109 | 10,768 | 105,267 | 10.12 | 1.04 |
| Total* | 7,133 | 901,504 | 8,882,190 | 7.91 | 0.8 |
*Total is less than total number of hospitalizations (7,310) because only patients residing in NJ counties are included in the table.
Geographic Injection-Related Severe Bacterial Infection (SBI) Trends
Overall hospitalizations for injection drug use-related infections were highest in Camden, Essex, & Passaic counties.
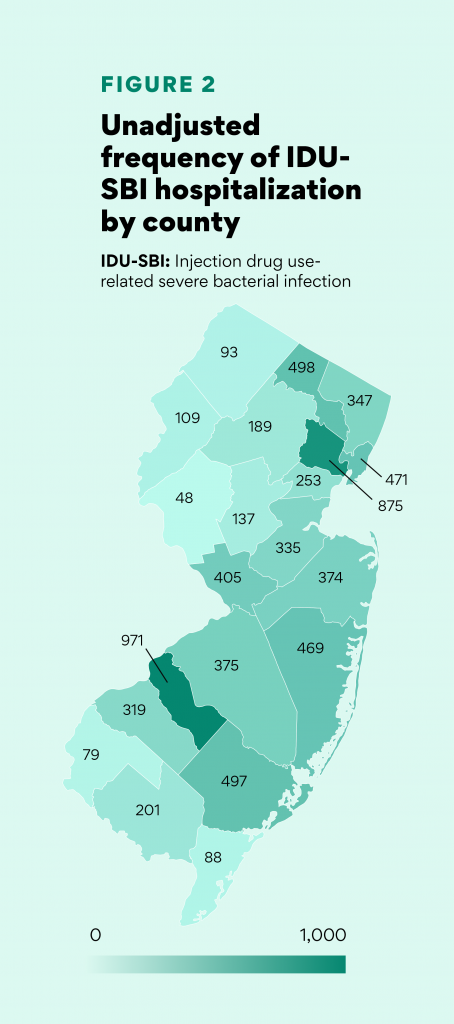
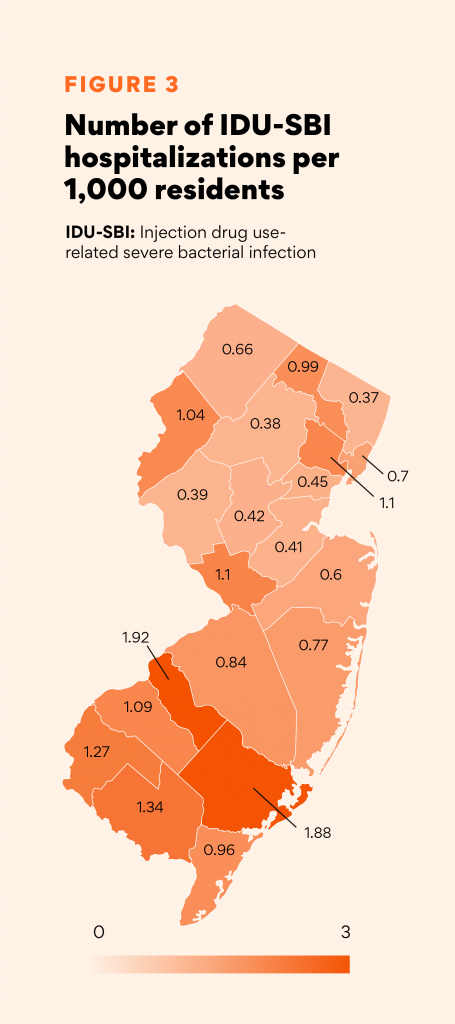

Counties with the highest rates per capita of hospitalizations due to preventable injection drug-use related SBIs were Atlantic, Camden, Cumberland, Mercer, and Salem.
Estimated Charges
Notably, charges for IDU-related infections account for 27.3% of charges for ED/inpatient visits in the state for injection-related SUDs (calculated at $3.7 billion total). This is the equivalent of community college tuition costs for over 160,000 residents or enough to fully fund at least two syringe service programs for every municipality in the state.
Charges for injection drug- use related infections total over $1.0 billion — enough to fully fund at least two syringe service programs in every municipality in the state.
FIGURE 5 Charge associated with visit by morbidity*
*Figure displays the charge for hospitalization associated with a visit of an indicated diagnosis. Box denotes the interquartile range with line showing the median. Whiskers display values at 1.5 times below and above the IQR. Values outside this range are hidden.
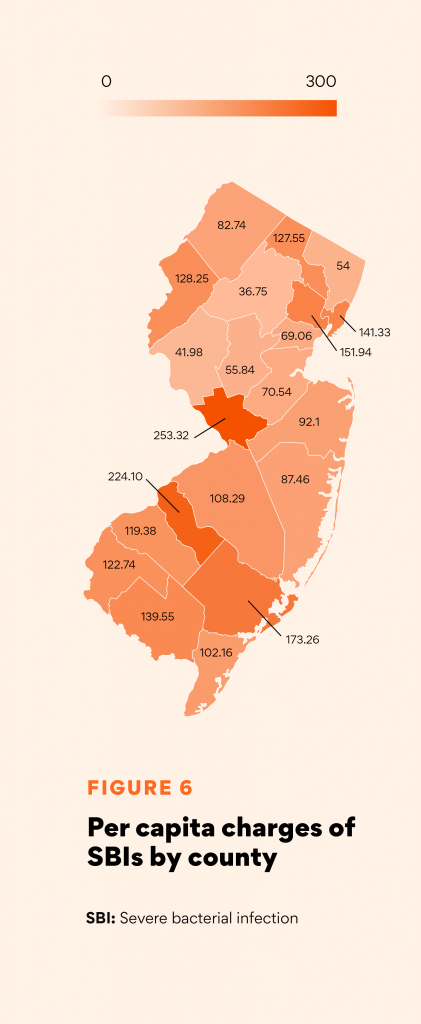
TABLE 3
IDU-SBI-associated charge per county (in dollars)
IDU-SBI: Injection drug use-related severe bacterial infection
| County | Mean | Median | Maximum | Total | Charges per Capita |
|---|---|---|---|---|---|
| Atlantic | 91,918 | 56,132 | 1,268,002 | 45,683,236 | 173.26 |
| Bergen | 145,064 | 78,021 | 2,975,607 | 50,337,124 | 54 |
| Burlington | 128,604 | 65,392 | 1,410,164 | 48,226,592 | 108.29 |
| Camden | 116,891 | 63,488 | 2,094,108 | 113,500,000 | 224.1 |
| Cape May | 106,844 | 54,003 | 1,502,626 | 9,402,299 | 102.16 |
| Cumberland | 103,815 | 51,042 | 1,618,692 | 20,866,780 | 139.55 |
| Essex | 138,730 | 70,819 | 3,408,917 | 121,400,000 | 151.94 |
| Gloucester | 109,136 | 68,191 | 953,120 | 34,814,252 | 119.38 |
| Hudson | 201,760 | 125,684 | 2,108,900 | 95,028,872 | 141.33 |
| Hunterdon | 108,763 | 57,192 | 1,311,067 | 5,220,601 | 41.98 |
| Mercer | 229,824 | 124,083 | 2,722,060 | 93,078,840 | 253.32 |
| Middlesex | 173,720 | 112,019 | 2,232,791 | 58,196,048 | 70.54 |
| Monmouth | 152,789 | 74,027 | 2,884,294 | 56,990,344 | 92.1 |
| Morris | 95,633 | 65,252 | 707,625 | 18,074,720 | 36.75 |
| Ocean | 113,227 | 68,198 | 1,266,227 | 53,103,664 | 87.46 |
| Passaic | 128,533 | 73,560 | 1,495,636 | 64,009,528 | 127.55 |
| Salem | 96,929 | 50,260 | 557,442 | 7,657,372 | 122.74 |
| Somerset | 134,072 | 91,260 | 1,058,524 | 18,367,792 | 55.84 |
| Sussex | 124,984 | 79,778 | 1,103,769 | 11,623,514 | 82.74 |
| Union | 151,852 | 84,848 | 1,555,779 | 38,418,608 | 69.06 |
| Warren | 123,853 | 81,369 | 865,222 | 13,500,025 | 128.25 |
| Total* | 2,776,941 | 1,594,618 | 35,100,572 | 977,500,211 | 2,382.34 |
Conclusion & Recommendations
Among New Jersey residents in 2019, our analysis found:
- 1,967 ED visits for IDU-SBIs
- 7,310 hospitalizations for IDU-SBIs, accounting for 0.8% of all hospitalizations and 15.2% of hospitalizations with an injection-related SUD diagnosis
- 283 in-hospital deaths from IDU-SBIs
- More than $1 billion in hospital charges due to IDU-SBIs, with a median charge of $74,406 per hospitalization
New Jersey currently operates only seven syringe service programs in a state with over nine million residents.
Each program serves an average of 1.29 million residents.
- Include prevalence of IDU-SBIs, as well as deaths related to such infections, in publicly available drug user health metrics. The prevalence and incidence of SBIs should be included in public data dashboards on the health outcomes faced by New Jerseyans who use drugs and who are living with an SUD.
- Fully fund and implement accessible syringe service programs in all corners of the state. Ensuring PWID have access to sterile syringes and other safer injection supplies is critical to preventing SBIs. New Jersey currently has only seven syringe services programs serving over nine million residents. In light of recent legislative changes to remove restrictive barriers to syringe access, New Jersey must fully fund and implement syringe exchange programs. New Jersey must also ensure that syringe access is accessible to all residents by increasing access through brick-and-mortar drop-in locations, delivery and mail-based services, and peer-led delivery models.
- Support harm reduction services that include safer smoking and safer snorting supplies to decrease IDU-related infections. Switching route of administration from injection to smoking or snorting reduces risk of overdose, SBIs, and trans-mission of HIV and Hepatitis C. Funding should be available for safer smoking and snorting supplies, and these supplies should be offered by all harm reduction programs. Criminal penalties should be removed for possession and distribution of these supplies in the interest of public health.
- Increase harm reduction infrastructure in EDs and hospitals. PWID often experience competing priorities that prevent them from accessing medical care, such as knowing they will experience withdrawal while hospitalized, the stigma associated with IDU, and knowing that infections could be life threatening if left untreated. All EDs and hospitals should have evidence-informed withdrawal management
(consisting primarily of medications for opioid use disorder) readily available for patients. Hospitals should provide connection to syringe service programs and prioritize collaborative care plans to address patient-identified needs and reduce the odds of patient-directed discharges. It is critical to increase local substance use treatment collaboration between hospitals and treatment centers for individuals who are seeking supported SUD treatment. - Decriminalize drug possession and use. SUD is a chronic health condition, expected symptoms of which include continuing to use despite negative consequences or the desire to stop. The criminalization of drug use decreases the likelihood that people who use drugs will seek medical care, and increases stigma and discrimination for those seeking medical care. Drug use is a matter of public health and community wellbeing; it should be treated as such.
- Provide training to healthcare providers to reduce stigma against people who use drugs. Studies have found that people who use drugs avoid medical care because of mistreatment by health care providers, often rooted in stigma.5 As a result, minor IDU-related infections may progress to serious and potentially fatal ones before individuals seek treatment. More education across health care sectors, especially for first responders, emergency providers, and providers in EDs, is needed to address stigma, promote equitable care, and better meet the medical needs of people who use drugs.
References
- Tookes H, Diaz C, Li H, Khalid R, Doblecki-Lewis S. A Cost Analysis of Hospitalizations for Infections Related to Injection Drug Use at a County Safety-Net Hospital in Miami, Florida. Paraskevis D, ed. PLoS ONE.2015;10(6):e0129360. doi:10.1371/journal.pone.0129360
- Capizzi J, Leahy J, Wheelock H, et al. Population-based trends in hospitalizations due to injection drug use-related serious bacterial infections, Oregon, 2008 to 2018. Zaller ND, ed. PLoS ONE. 2020;15(11):e0242165. doi:10.1371/journal.pone.0242165
- Office of the Chief State Medical Examiner. Drug-Related Death Dashboard. Official Site of the State of New Jersey. Published February 21, 2022. Accessed February 26, 2022. https://ocsme.nj.gov/Dashboard?_gl=1*crrwcf*_ga*MTcxMDg2Nzk5Ni4xNjQyMDI0M-DUx*_ga_5PWJJG6642*MTY0NTkwMjAzOC4zLjEuMTY0NTkwMjA2My4w
- Mellor J. A War on Us: How Much New Jersey Spends Enforcing the War on Drugs. New Jersey Policy Perspective; 2021. Accessed September 30, 2021.https://www.njpp. org/publications/report/a-war-on-us-how-much-new-jersey-spends-enforcing-the-war-on-drugs/
- Meyerson BE, Russell DM, Kichler M, Atkin T, Fox G, Coles HB. I don’t even want to go to the doctor when I get sick now: Healthcare experiences and discrimination re-ported by people who use drugs, Arizona 2019. International Journal of Drug Policy. 2021;93:103112. doi:10.1016/j.drugpo.2021.103112
- Binswanger IA, Kral AH, Bluthenthal RN, Rybold DJ, Edlin BR. High Prevalence of Abscesses and Cellulitis Among Community-Recruited Injection Drug Users in San Francis-co. Clinical Infectious Diseases. 2000;30(3):579-581. doi:10.1086/313703
- Damlin A, Westling K. Patients with infective endocarditis and history of injection drug use in a Swedish referral hospital during 10 years. BMC Infect Dis. 2021;21(1):236. doi:10.1186/s12879-021-05914-1
- Thakarar K, Rokas KE, Lucas FL, et al. Mortality, morbidity, and cardiac surgery in Injection Drug Use (IDU)-associated versus non-IDU infective endocarditis: The need to expand substance use disorder treatment and harm reduction services. West B, ed. PLoS ONE. 2019;14(11):e0225460. doi:10.1371/journal.pone.0225460
- Waltenburg MA, Larson V, Naor E, et al. Notes from the Field: Botulism Type B After Intravenous Methamphetamine Use — New Jersey, 2020. MMWR Morb Mortal Wkly Rep. 2020;69.doi:10.15585/mmwr.mm6939a4
- Philadelphia Department of Public Health. Hospitalizations for Infections Related to Injection Drug Use, 2013–2018. 5(1):1-6.
- Weiss AJ, Stocks C. Hospital Inpatient Stays Related to Opioid Use Disorder and Endocarditis, 2016. https://www.hcup-us.ahrq.gov/reports/statbriefs/sb256-Opioids-Endocarditis-Inpatient-Stays-2016.jsp
- Ronan MV, Herzig SJ. Hospitalizations Related To Opioid Abuse/Dependence And Associated Serious Infections Increased Sharply, 2002–12. Health Affairs. 2016;35(5):832-837.doi:10.1377/hlthaff.2015.1424
- Healthcare Cost and Utilization Project (HCUP). Opioid Hospital Stays/Emergency Department Visits – HCUP Fast Stats. Agency for Healthcare Research and Quality; 2021. Accessed January 1, 2022. https://www.hcup-us.ahrq.gov/faststats/OpioidUseServlet
- Barocas JA, Gai MJ, Amuchi B, Jawa R, Linas BP. Impact of medications for opioid use disorder among persons hospitalized for drug use-associated skin and soft tissue infections. Drug and Alcohol Dependence. 2020;215:108207. doi:10.1016/j. drugalcdep.2020.108207
- U.S. Census Bureau, Population Division. Annual Estimates of the Resident Population for Counties in New Jersey: April 1, 2010 to July 1, 2019 (CO-EST2019ANNRES-34); 2020.
- Ti L, Ti L. Leaving the Hospital Against Medical Advice Among People Who Use Illicit Drugs: A Systematic Review. Am J Public Health. 2015;105(12):e53-e59. doi:10.2105/AJPH.2015.302885
- Kimmel SD, Kim JH, Kalesan B, Samet JH, Walley AY, Larochelle MR. Against Medical Advice Discharges in Injection and Non-injection Drug Use associated Infective Endocarditis: A Nationwide Cohort Study. Clinical Infectious Diseases. 2021;73(9):e2484-e2492. doi:10.1093/cid/ciaa1126
- Syringe Services Programs (SSPs) Fact Sheet | CDC. Published July 24, 2019. Accessed January 1, 2022. https://www.cdc.gov/ssp/syringe-services-programs-factsheet.html
- HIV, STD, and TB Services. Harm Reduction Centers. NJ Department of Health. Accessed January 1, 2022. https://www.nj.gov/health/hivstdtb/sap.shtml
- Office of Planning, Research, Evaluation, Prevention and Olmstead. Substance Abuse Overview Statewide Report – 2019. Department of Human Services Division of Mental Health and Addiction Services; 2020.
Appendix
ICD-10 Diagnosis Codes
The following ICD-10 codes were used to identify hospital visits indicative of infections associated with injection drug use. ICD-10 codes were determined through a review of prior literature, which is cited below for each condition.
*Denotes use of all subsequent ICD-10 codes.
Substance Use-Related Codes2,12
| T40.0X1* | Poisoning by opium, accidental (unintentional) | |
| T40.0X2* | Poisoning by opium, intentional self-harm | |
| T40.0X3 | Poisoning by opium, assault | |
| T40.0X4* | Poisoning by opium, undetermined | |
| T40.0X5* | Adverse effect of opium | |
| T40.1X* | Poisoning by and adverse effect of heroin | |
| T40.2X1* | Poisoning by other opioids, accidental (unintentional) | |
| T40.2X2* | Poisoning by other opioids, intentional self-harm | |
| T40.2X3* | Poisoning by other opioids, assault | |
| T40.2X4* | Poisoning by other opioids, undetermined | |
| T40.2X5* | Adverse effect of other opioids | |
| T40.3X1* | Poisoning by methadone, accidental (unintentional) | |
| T40.3X2* | Poisoning by methadone, intentional self-harm | |
| T40.3X3* | Poisoning by methadone, assault | |
| T40.3X4* | Poisoning by methadone, undetermined | |
| T40.3X5* | Adverse effect of methadone | |
| T40.4X1* | Poisoning by other synthetic narcotics, accidental (unintentional) | |
| T40.4X2* | Poisoning by other synthetic narcotics, accidental (unintentional) | |
| T40.4X3* | Poisoning by other synthetic narcotics, assault | |
| T40.4X4* | Poisoning by other synthetic narcotics, undetermined | |
| T40.4X5* | Adverse effect of other synthetic narcotics | |
| T40.411* | Poisoning by fentanyl or fentanyl analogs, accidental | |
| T40.412* | Poisoning by fentanyl or fentanyl analogs, self-harm | |
| T40.413* | Poisoning by fentanyl or fentanyl analogs, assault | |
| T40.414* | Poisoning by fentanyl or fentanyl analogs, undetermined | |
| T40.415* | Adverse effect of fentanyl or fentanyl analogs | |
| T40.421* | Poisoning by tramadol, accidental (unintentional) | |
| T40.422* | Poisoning by tramadol, intentional self-harm | |
| T40.423* | Poisoning by tramadol, assault | |
| T40.424* | Poisoning by tramadol, undetermined | |
| T40.425* | Adverse effect of tramadol | |
| T40.491* | Poisoning by other synthetic narcotics, accidental | |
| T40.492* | Poisoning by other synthetic narcotics, self-harm | |
| T40.493* | Poisoning by other synthetic narcotics, assault | |
| T40.494* | Poisoning by other synthetic narcotics, undetermined | |
| T40.495* | Adverse effect of other synthetic narcotics | |
| T40.601* | Poisoning by unspecified narcotics, accidental (unintentional) | |
| T40.602* | Poisoning by unspecified narcotics, intentional self-harm | |
| T40.603* | Poisoning by unspecified narcotics, assault | |
| T40.604* | Poisoning by unspecified narcotics, undetermined | |
| T40.605* | Adverse effect of unspecified narcotics | |
| T40.691* | Poisoning by other narcotics, accidental (unintentional) | |
| T40.692* | Poisoning by other narcotics, intentional self-harm | |
| T40.693* | Poisoning by other narcotics, assault | |
| T40.694* | Poisoning by other narcotics, undetermined | |
| T40.695* | Adverse effect of other narcotics | |
| F11* | Opioid related disorders | |
| F13* | Sedative, hypnotic, or anxiolytic related disorders | |
| F14* | Cocaine related disorders | |
| F15* | Other stimulant related disorders | |
| F19* | Other psychoactive substance related disorders |
Endocarditis10
| M32.11 | Endocarditis in systemic lupus erythematosus |
| A32.82 | Listerial endocarditis |
| A39.51 | Meningococcal endocarditis |
| A52.03 | Syphilitic endocarditis |
| A54.83 | Gonococcal heart infection |
| B37.6 | Candidal endocarditis |
| I01.1 | Acute rheumatic endocarditis |
| I33.0 | Acute and subacute infective endocarditis |
| I33.9 | Acute and subacute endocarditis, unspecified |
| I38 | Endocarditis, valve unspecified |
| I39 | Endocarditis and heart valve disorders in diseases classified elsewhere |
Bacteremia and Sepsis2
| A40* | Streptococcal sepsis |
| A41* | Other sepsis |
| I26.90 | Septic pulmonary embolism without acute cor pulmonale |
| I40.0 | Infective myocarditis |
| I76 | Septic arterial embolism |
| R65.10 | SIRS of non-infectious origin w/o acute organ dysfunction |
| R65.20 | Severe sepsis without septic shock |
| R65.21 | Severe sepsis with septic shock |
| R78.81 | Bacteremia |
Osteomyelitis2
| M46.2* | Osteomyelitis of vertebra |
| M46.3* | Infection of intervertebral disc (pyogenic) |
| M86.1* | Other acute osteomyelitis |
| M86.2* | Subacute osteomyelitis |
| M86.9 | Osteomyelitis, unspecified |
Skin and Soft Tissue Infections13
| A48.0 | Gas gangrene |
| I80.0* | Phlebitis and thrombophlebitis of superficial vessels of low extremities |
| I80.1* | Phlebitis and thrombophlebitis of femoral vein |
| I80.21* | Phlebitis and thrombophlebitis of iliac vein |
| I80.22* | Phlebitis and thrombophlebitis of popliteal vein |
| I80.23* | Phlebitis and thrombophlebitis of tibial vein |
| I80.29* | Phlebitis and thrombophlebitis of deep vessels of low extremities |
| I80.3 | Phlebitis and thrombophlebitis of lower extremities, unspecified |
| I80.8 | Phlebitis and thrombophlebitis of other sites |
| I80.9 | Phlebitis and thrombophlebitis of unspecified site |
| L02* | Cutaneous abscess, furuncle and carbuncle |
| L03 | Cellulitis and acute lymphangitis |
| M54.02* | Panniculitis affecting regions of neck/bk, cervical region |
| M72.6* | Necrotizing fasciitis |
| M79.3* | Panniculitis, unspecified |
Donate Now
Harm reduction is essential. A harm reduction approach to drug use is the best strategy we have to end the overdose crisis, reduce risks associated with drug use, and affirm the dignity and bodily autonomy of every New Jerseyan.


